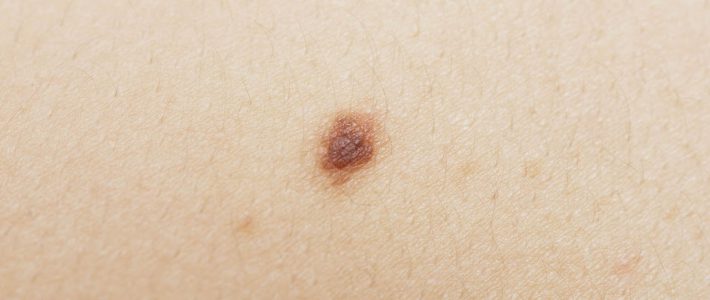
Cancer is the main cause of mortality in Canada. According to the Canadian Cancer Society, over 7200 Canadians will be diagnosed with melanoma in 2017 [1]. Chances of survival are enhanced if the tumor is quickly discovered, yet melanoma remains a highly aggressive cancer in advanced stages [2]. Everyone, including aestheticians, can play a key role in the prevention of melanoma by knowing how to identify its precursors. This guide is developed to help you identify those suspicious precursors in one quick glance.
Following a physiological imbalance, melanocytes multiply in an uncontrollable manner creating a new precancerous spot or modifying pre-existing beauty marks, which can then transform into melanoma. Detecting suspicious spots or beauty marks is a measure of prevention. Three types of precancerous spots can be observed [3] [4] [5]:
- Dysplastic Nevus (atypical beauty mark)
- Congenital Melanocytic Nevi (atypical beauty mark or birthmark)
- Lentigo Maligna
Most often, these beauty marks never reach a cancerous state but they are predisposing factors to the development of a melanoma [6] [7]. Lentigo maligna is considered today a very precancerous form of melanoma [5].
- Dysplastic Nevus
A brown or reddish-brown beauty mark with an irregular shape and undefined borders, the dysplastic nevus is larger than a classical mole, measuring more than 6 mm. Particular attention should be paid to their number. The higher their number, the higher is the risk to develop melanoma [7] [8].
- Congenital Melanocytic Nevi
The congenital melanocytic nevi appears at birth or during childhood as a beauty mark or mole. Its size can vary between 1.5 cm to 20 cm and larger in certain cases. The risk of developing melanoma is proportional to the size of nevi [7] [9].
- Lentigo Maligna
Chronically exposed to sun, some areas of the skin can be marked by ocher to brown colored flat spots [5]. These may be simple lentigo or malignant lentigo which are hard to distinguish from one another. The presence of lentigo maligna marks the beginning of a precancerous melanoma. High sun exposure increases the risk of lentigo maligna development on the skin. Although most people affected by these marks are advanced in age, lentigo maligna is increasingly observed on young adults [10].
To simplify the detection of a precancerous mark, the ABCDE rule exists. It is about meticulous observation of the beauty spot by noting the following [11]:
- A for Asymmetry: note if the shape is regular or not. If half the spot has a shape different than the other half, asymmetry is present.
- B for irregular Border: note if the edge of the beauty mark or spot is blurred.
- C for varied Colours: observe the coloring of the beauty mark which could range from light brown to dark. Sometimes, colors such as blue, grey, red, pink or white may be found.
- D for Diameter: check if the beauty mark measures more than 6 mm.
- E for Evolution: note the change of size, color, shape or texture of the beauty mark with time. Inquire about sensations felt such as itching, burning or tingling.
If one or several of these criteria is noticed, it is important to advise your client to see a doctor [11].
In light of the devastation cancer is today, the smallest observation of a suspicious marking on the skin can save lives…
Internet Sources:
[1] http://www.cancer.ca/en/cancer-information/cancer-type/skin-melanoma/statistics/?region=on
[7] http://www.cancer.ca/en/cancer-information/cancer-type/skin-melanoma/risks/?region=on#atypicalmoles
[9] https://www.cancer.org/cancer/melanoma-skin-cancer/causes-risks-prevention/risk-factors.html
[11] http://www.cancer.ca/en/cancer-information/cancer-type/skin-melanoma/signs-and-symptoms/?region=on
Bibliography:
[3] Le mélanome, un guide de la Ligue contre le cancer pour les personnes atteintes et leurs proches.
[4] Melanoma, Guidelines for patients, National Comprehensive Cancer Network
[6] Meenhard Herlyn, Dorothée Herlyn, David E. Elder, Edward Bondi, Donato LaRossa, Ralph Hamilton, Henry F. Sears, Gloria Balaban, DuPont Guerry IV, Wallace H. Clark, and Hilary Koprowski, (1983) Phenotypic Characteristics of Cells Derived from Precursors of Human Melanoma, Cancer Research 43, 5502-5508
[8] Alisa M. Goldstein, Margaret A. Tucker, (2013) Dysplastic Nevi and Melanoma, Cancer Epidemiol Biomarkers Prev.; 22(4): 528–532
[10] Frédérique-Anne Le Gal, Laurence Toutous-Trellu, Gürkan Kaya et Denis Salomon, (2011) Lentigo maligna: un mélanome particulier, Rev Med Suisse; 7 : 765-71